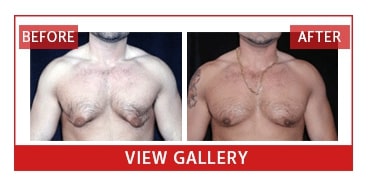
Many people have questions about Gynecomastia, what is looks likes, what can cause it, and how can it be treated. Dr. Rick Silverman has provided some of the most frequently asked questions about Gynecomastia to help you better understand this condition.
What Does Gynecomastia Look Like?
Gynecomastia can look like women’s breasts, but that would be a very extreme case. In most cases it starts as a little lump under the nipple, usually during puberty. The lump usually goes away with time, but not always. Sometimes it gets bigger, causing the nipple to stick out. In a boy who is a little overweight, the chest might really start to look more like his sister’s chest with early breast development. Some kids can even squeeze a little fluid out of the nipple.
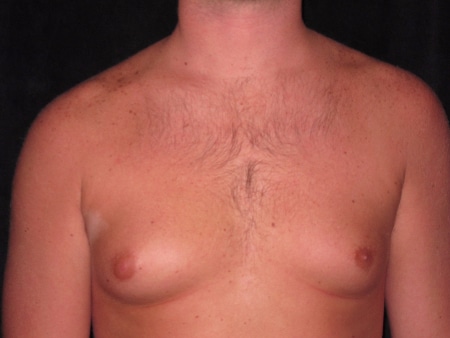
It’s a pretty frightening experience for an adolescent, so lots of guys just ignore it hoping it will go away–unless their parents push them into seeing their doctor.
Is Gynecomastia Common?
A number of studies have looked at the frequency of gynecomastia in the general population, and the incidence may be as high as 60 – 70%. What is found is that it occurs most commonly in three age groups: newborns, boys during puberty, and older men.
The bottom line with gynecomastia is that it occurs due to an abnormality in the ratio of testosterone to estrogens in the body. When this ratio is low, the estrogen effect is stronger and stimulates the growth of the tissue around the breast. The testosterone which is most important is not bound to protein in the blood, in other words, the free serum testosterone. This has been found to be lower in boys with gynecomastia compared to those without, while all the other hormone levels were about the same.
Gynecomastia In Newborns And Older Men
More or less the same things are happening to cause gynecomastia, but for different reasons. In newborns, there are lots of maternal hormones floating around, so the breast tissue may be stimulated by them. In older men, the testosterone production usually decreases, so the ratio is lowered and allows for stimulation of the breast tissue by estrogens. Next thing you know, it’s time to go shopping for your “manziere”.
Does The Tissue Look Like Women’s Breast Tissue?
It does to a certain extent, in that it is made up of ducts, fat and other elements which are found in women’s breasts. At the same time, it looks different to a pathologist who is looking at the tissue under a microscope–it doesn’t really form glands to make milk as it does in women.
Why Would A Pathologist Look At The Tissue? Is This A Type Of Cancer?
No, Gynecomastia is not cancer. It is a benign disease and can be a real bummer for a guy who gets it. In any case, a lump in the breast should always cause some concern. Breast cancer in men is very unusual and happens less than 1% and is generally in older men. Gynecomastia often occurs on both sides, so if a breast mass occurs on only one side, it may be more suspicious for cancer. It would be extremely unusual to see male breast cancer on both sides at the same time.
Sometimes a patient’s history may give a clue as to whether or not the lump could be cancer. In other cases, a mammogram or ultrasound may be required. Sometimes a biopsy of the tissue must be done to be sure it isn’t cancer. Although needle biopsies, which just take a small sample of tissue, may suggest that the lump is cancer, the only way to confirm that it is not cancer is to cut out the entire mass and examine it under a microscope.
If It’s Not Cancer, What Are The Next Steps?
The presence of gynecomastia can be a sign of other problems, such as a hormonally active tumor in the testicle, adrenal glands, or brain, most commonly. Clearly, excision of the gynecomastia will not be adequate treatment in these patients, who still need treatment for their primary problem. One of my patients had cancer of his adrenal gland which produced estrogen and left him with a couple of C-cup breasts. Two years after his initial treatment, his gynecomastia was worsening, and they discovered recurrence of his tumor, which required further cancer treatment. Consideration must be given to these other, potentially life-threatening problems, which can usually be ruled out based on history and additional hormone studies. A simple examination of the testicles, or possibly an ultrasound study, can be life-saving.
Can Gynecomastia Turn In To Cancer?
Cancer arising in gynecomastia has been described in the medical literature, but it is very uncommon. Otherwise, everyone with gynecomastia would be encouraged to have it removed as a preventative measure. In fact, that isn’t the case.
Gynecomastia And Steriods
All of these hormones I’ve been talking about are steroids. In bodybuilding and other sports, anabolic steroids, which are taken to enhance performance, may cause gynecomastia as a side effect. The ones that are most commonly associated with this problem are those which undergo “aromatization”, or conversion to estrogen-like compounds, a process which takes place in fat and muscle cells. These estrogens cause a shift in that ratio I mentioned earlier, leading to growth of the breast tissue. The testosterones and anadrol are common culprits, but some of the other testosterone derivatives can be responsible as well.
Androgens And The Impact On Your Body
Someone can be taking androgens to become more manly and instead he can end up with breasts. The testosterone levels are much higher than normal, so for the most part, the estrogens cause some mild side effects which are mostly just an inconvenience. In the case of gynecomastia, though, the local effect is such that the change in the ratio is enough to lead to development of this problem. Interestingly, it is most noticeable as the user comes off from a cycle of steroids. The reason for that is that the body slows down it’s own testosterone production when the drugs are being used. It takes a little while for the testes to kick in and start making normal amounts of testosterone, so the ratio is way off for a short while, leading to extra stimulation of that breast tissue.
When A Guy Is Off A Cycle, Could He Expect The Breast Tissue To Decrease?
The extra stimulation may go away, yes, but the tissue doesn’t necessarily return to normal. In fact, usually it doesn’t. Over time, with additional drug cycles, the tissue builds up. with an accumulation of glandular tissue mixed with fat and scar tissue. This tissue is mostly under the areola–that’s the dark skin around the nipple. In the off-season, when a bodybuilder’s bodyfat is higher, the problem may be masked if it’s minor. If it’s severe, the chest may take on a truly female-like appearance, and the nipples frequently point downward.
Is There A Way To Predict Who Will Get Gynecomastia?
The only thing he got out of his brief cycle–was a case of Gynecomastia. As mild as it was, he was psychologically wrecked by it.
If You Know That Aromatization Of Steroids Can Lead To Gynecomastia, Can You Prevent This Process Or Treat It With Medicine?
Obviously, the first means of prevention is to not use steroids. The alternative, which many steroid users take, is to use agents which undergo less or no aromatization. An alternative to that approach, is the use of agents which block estrogen, such as Tamoxifen (Nolvadex) or Arimidex, or drugs which block aromatization. Proviron and Testolactone are two drugs which bind to the enzyme “aromatase” to prevent it from working. These drugs may be effective in preventing this side effect, if they are taken before it happens. You have to understand, though, that this has never been studied in athletes who use steroids. The information is basically anecdotal. The use of Tamoxifen has been shown to be effective in patients with hormonally active tumors. And there are newer drugs on the horizon which may be more effective with fewer down sides. As for drugs which can make the gynecomastia go away–well, there aren’t any so far.
What About Some Of The More Recent Products On The Market That Claim To Increase Testosterone Levels–hormones Such As Androstenedione, Dhea And Similar Compounds?
These Hormones Are Basically Testosterone Precursors, So Is It Possible For Them To Cause Gynecomastia?
These hormones are androgens, and they can also be converted to estrogens. It’s hard to find information on the amounts converted, but it turns out that Christopher Longcope, M.D., one of the pioneers in sex-steroid research, had his office down the hall from my office at the University of Massachusetts. I asked him about this issue specifically, since I was curious to know how safe these supplements were, for my own use and so that I could tell my patients. His feeling was that the risk is quite low. He bases his opinion on the fact that only small amounts of each ingested dose are actually converted to testosterone, like 0.4% and even smaller amounts are aromatized. Of course this also means that there’s as good as no chance for this stuff to actually make you bigger and stronger. Nonetheless, I have seen a few patients who feel that they developed gynecomastia related to use of these products.
Read what our patients are saying!
"I spent a good portion of my 20’s suffering from Gynecomastia. In 2010 I reached out to Dr. Rick Silverman for a consultation. It was the best money I ever invested in myself."
Click here to read more reviews.
Can Drugs Other Than Steroids Cause Gynecomastia?
Sure. One of the questions I ask my gynecomastia patients who don’t use steroids is if they smoke marijuana. And I bet that lots of steroid users have confessed marijuana use before they’d admit to steroid use at the doctor’s office. Other prescription drugs which are associated with the condition include the anti-ulcer drug, cimetidine or “Tagamet”, and Spironolactone, which is a diuretic used for high blood pressure. Another agent that we tend to forget about is alcohol, which can affect metabolism in the liver, enhancing the effect of other drugs as well as contributing to development of gynecomastia itself.
Can Gynecomastia Develop From The Use Of A Testosterone Patch?
If you review the guidelines for the patch, gynecomastia is listed as a potential side effect, but it is rarely observed. In fact, you have the theoretical advantage of increased levels of testosterone leading to a better ration to estrogen and preventing the development of gynecomastia in older men.
Is Surgery The Only Option To Treat Gynecomastia?
Yes. In most cases, the surgery can be performed as an outpatient procedure, using local anesthesia with some sedation or a light general anesthetic. The surgeon may cut out the “tumor” directly, going through an incision along the edge of the areola, or liposuction may be used. When direct excision is used, a button of tissue must be left under the nipple to prevent it from dying due to loss of its blood supply, and also to keep it from caving in and leaving a depression on the chest wall.
Liposuction Vs. Excision
Liposuction is a great tool when the condition is mostly caused by fatty tissue, because this is easily removed this way. In steroid related gynecomastia, the tissue under the nipple can be very dense, and I find that this must be cut out. Frequently, a combination of the two approaches is most effective, especially when I’m treating steroid-related disease. In my experience, this gives the best contour after surgery.
Are There Medical Reasons For Operating On Gynecomastia?
The biggest medical reason to evaluate abnormal growth in the breast is to rule out the potential for cancer. If this is unlikely, medical factors are less significant. In some patients, however, the pain associated with gynecomastia is fairly severe and this can be improved.
Are There Other Risks With Gynecomastia Surgery?
Problems which can occur include bleeding or hematoma formation, which can require a second operation for drainage of the collection of blood. This is more common in steroid users due to the high degree of vascularity of the chest wall. Infections are very unusual. The nipple sensation is usually altered after the operation, and in rare instances the nipple loses it’s blood supply and dies. In this case, it has to be removed and replaced as a skin graft, but it doesn’t look great when this is done. Depressions or contour irregularities can also occur.
Once You’ve Removed The Lump, What’s The Likelihood Of It Returning?
Well, remember that button of tissue I talked about–the tissue I leave under the nipple. That tissue contains the same elements which can be stimulated again if, for example, a guy starts taking steroids again. So it can come back. Interestingly, one of the first patients I operated on is a fellow who was in his early 40’s when I did his surgery. He hadn’t used steroids for about 5 years. His surgery went well. I did a little touch up liposuction of his chest the following year, and then I didn’t see him for a couple of years. When he showed up next time, he had bigger breasts than he’d had the very first time I saw him. After making sure that nothing else was wrong with him, it seemed that the likely cause of his recurrence was his dropping testosterone levels associated with aging. He was a victim of his own body’s hormonal back-fire.
What Are Some Of The Biggest Concerns Your Patients Have Undergoing Treatment For Gynecomastia?
You’d think it would be this issue of recurrence, but actually, because so many of my patients are involved in bodybuilding and fitness activities, their biggest worry is when they can get back to training. Every patient is different, of course, and many surgeons approach this issue differently, but I follow some general guidelines. Because the risk of bleeding following surgery in bodybuilders may be higher than in non-bodybuilders, it’s important for them to take it easy for about a week after the procedure. I limit my patients to light exercises, where they don’t get their blood pressure up–where they don’t sweat, basically. The second week, they can start sweating with cardio, and after two weeks they can start lifting weights.
When Can Patients Start Training Again?
I recommend that patients avoid training chest for four weeks. They should start that third week with light weights, maybe machines, even, just to get the blood flowing and so on. Gradually, heavier weights can be used. By not training chest for three or four weeks, they can avoid development of a fluid collection or other problem in the are of the surgery. After that, they should start back in slowly to avoid injury. Most patients are back to normal six weeks after their surgery, but their sanity has been maintained since they’ve been training all along.
Insurance: “To pay or not to pay….”
Does Insurance Pay For Your Gynecomastia Surgery?
Depending on where you live and what type of insurance you have, probably not. There are plenty of horror stories to be told relating to managed care, and a few of mine relate to Gynecomastia patients.
One young 13 year old was referred to my office by his primary care physician, a little large statured for his age, but not overweight and otherwise healthy. In his clothes, he looked like every other 13 year old, but when his shirt came off, he had small breasts which could have rivaled his sister’s. His condition had been stable for a couple years, suggesting that it was not likely to resolve without surgery. Typically, he was embarrassed and hesitant to take his shirt off in public. Sounds like something insurance ought to pay to remedy?
He Was Denied Coverage, And When Inquiry Was Made, The HMO Had A Single Indication For Which They Would Pay For Gynecomastia Surgery–suspected Cancer.
A few months later, a gentleman in his 50s came in with C-cup breast development following two surgeries and additional treatment for cancer of the adrenal glands. He was cured of his cancer, but he was terribly upset by the appearance of his chest. He received pre-approval to undergo a procedure to correct his gynecomastia, but when the bill for the surgeon’s fee was submitted for payment, no payment was made. Despite appeals and a hearing, the insurer–Medicaid, in this case–refused payment on the grounds that the procedure was cosmetic, even though it was a part of the treatment for his cancer.
With cases of insurance denial like these, don’t be surprised if your surgeon suggests that you pay out of pocket for your surgery, rather than experience the frustration of the insurance run-around.
Schedule A Consultation
Whatever the cause of gynecomastia–whether it’s caused by internal hormonal acrobatics or external forces like anabolic steroids, the condition is upsetting and it’s unsightly. In the case of bodybuilders, it may represent the “scarlet letter” of steroid use in individuals who are striving to create the best physique they possibly can. Obviously, avoiding the use of drugs will prevent many cases, but not all. The good news is that the condition can be treated safely and effectively. For more information or to schedule a consultation, call the office of Dr. Rick Silverman at (617) 965-9500.